Pacemaker Troubleshooting
Case 1
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
DDI
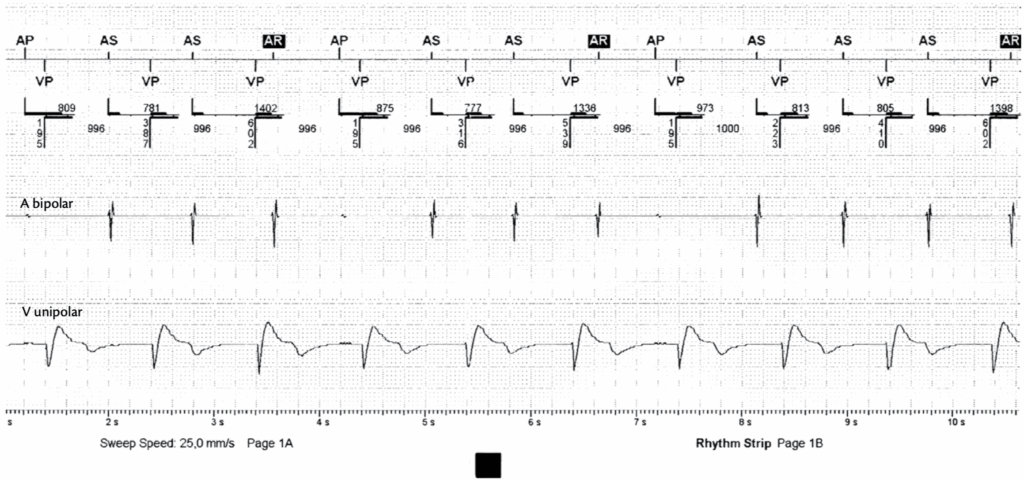
1 – There is loss of AV synchrony with atrial sensed events (AS) at a constant ventricular pacing (VP) rate 60 bpm (VP-VP 996 – 1000 ms) -> this excludes DDD and VDD.
2 – In DDI mode -> VA interval is triggered after a VP or VS events. AR that fall within the PVARP do not inhibit AP.
3 – AP occurs at the end of the VA interval (800 ms).
4 – AV synchrony is maintained after AP events.
Pros :
– To avoid to programme very long AV delays in the DDD mode, to avoid RV pacing
– Atrial tachy-arrhythmias, to avoid rapid ventricular pacing
Cons :
– Asynchrony
Case 2 An 82-year-old woman had been implanted with a single-chamber ventricular pacemaker 6 years ago for atrial fibrillation (AF) with symptomatic bradycardia. She presented to the hospital with shortness of breath and twitching of the left pectoral region. Her pacemaker follow-up, performed 6 months ago, had been completely normal. The results of the device follow-up performed at that time are shown here, and the electrocardiogram (ECG) recorded at admission.
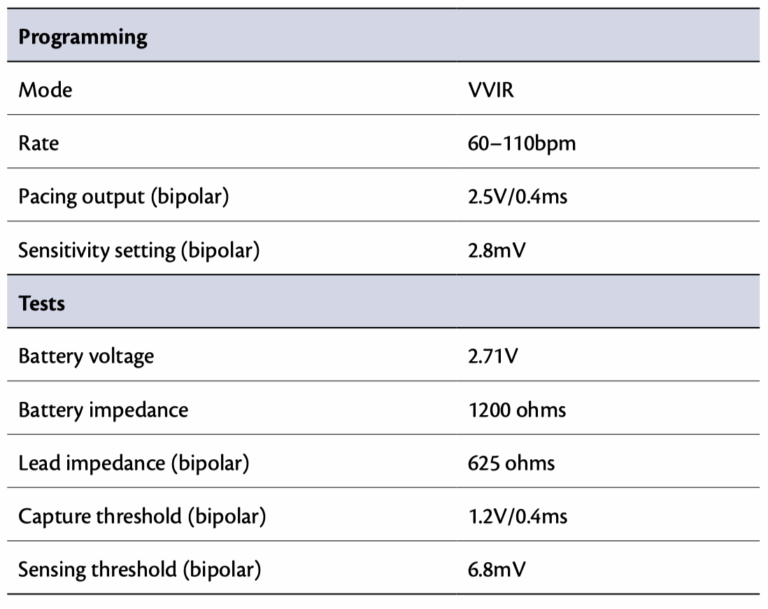
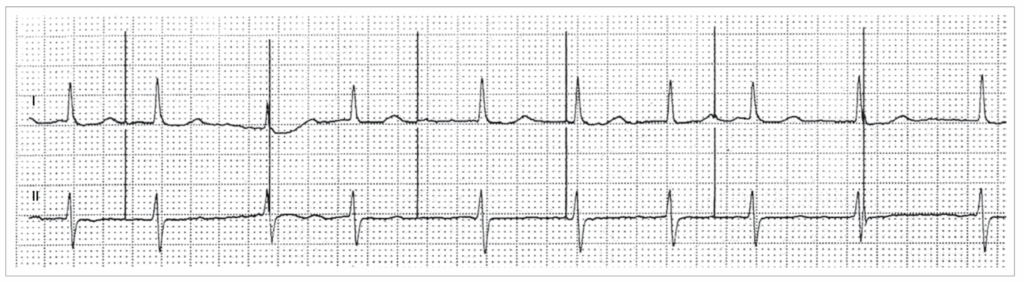
Ventricular undersensing
The pacing occur at 60 bpm (baseline rate) with under sensing & non capture
non capture is different from non pacing, non pacing is the lack of delivery of a pacing spike where one is expected.
Here we see a subclavian crush at the X-ray -> here we have a complet lead section due to subclavian crush
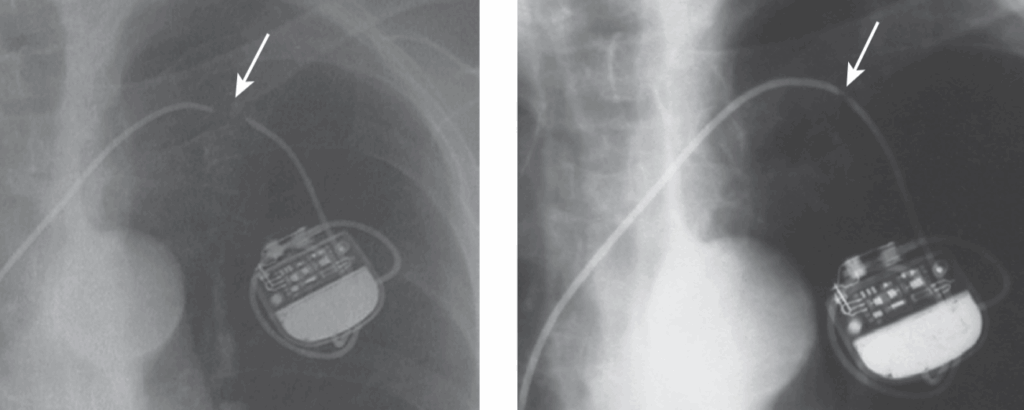
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 3
An 82-year-old patient with ischaemic heart disease and mildly reduced left ventricular ejection fraction (LVEF) was implanted, 1 month ago, with a St-Jude Medical singlechamber pacemaker for AF and symptomatic bradycardia.
The pacemaker was programmed to VVIR 60–110bpm.
The presenting EGM at follow-up is shown here
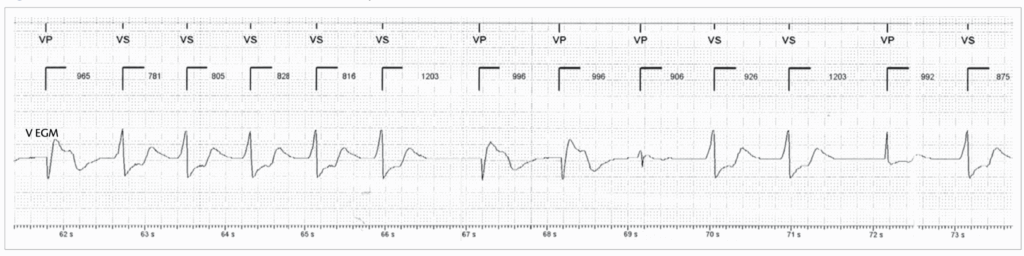
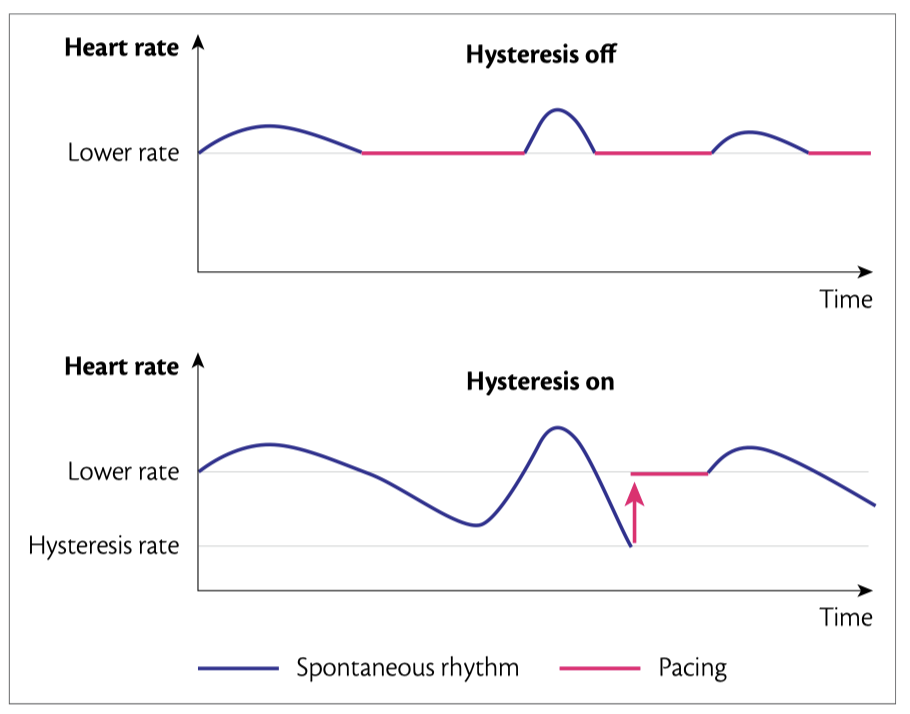
Rate Hysteresis
The device is programmed at a baseline rate of 60 bpm and a Rate hysteresis of 50 bpm
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 4
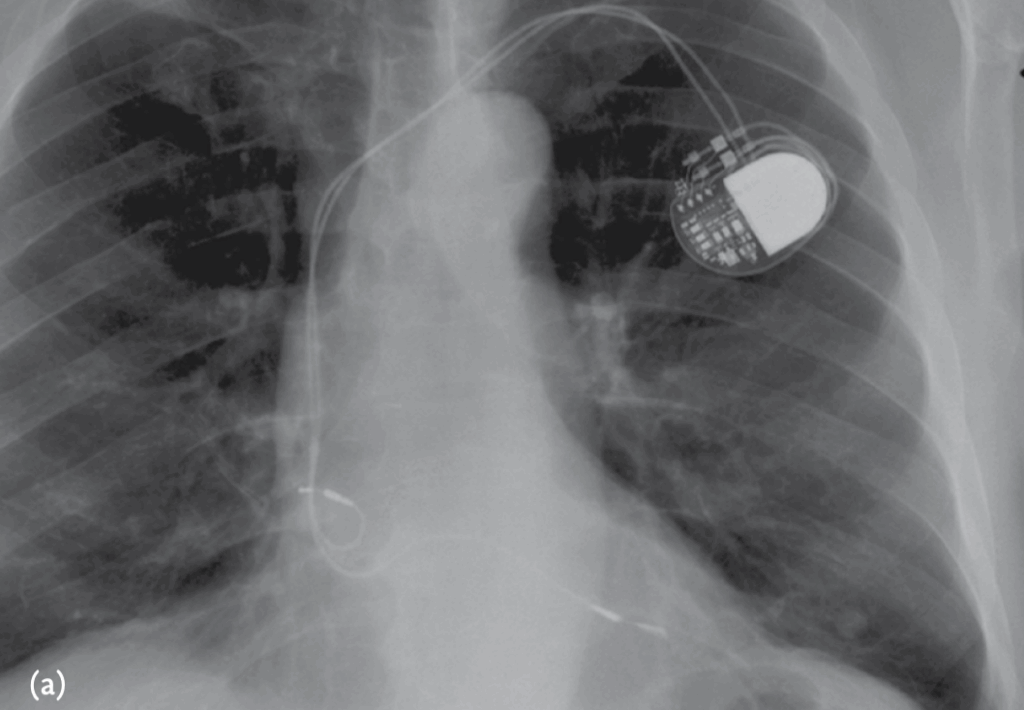
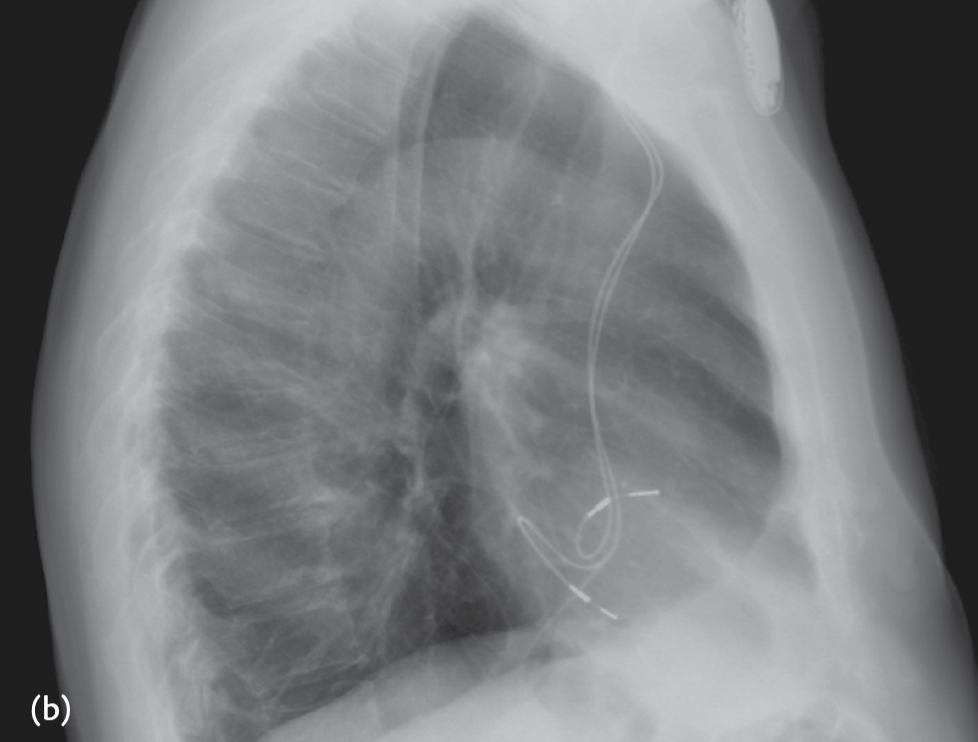
A 72-year-old patient was admitted for stroke. He had been implanted with a dual-chamber pacemaker 2 months ago for sinus dysfunction. Interrogation of the pacemaker was normal and did not disclose any atrial arrhythmias that may have explained the neurological event. A chest X-ray was performed and is shown
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
The ventricular lead is in the LV via a patent foramen ovale
- The PA view the ventricular lead would be expected in a lower position
- The lateral view shows the V lead to be posterior, whereas an RV lead would be anteriorly located.
- LV capture results in a negative QRS in lead I (which may be observed occasionally also with RV pacing) and an RBBB QRS morphology.
Case 5
An atrial threshold test was performed in a patient with sinus node dysfunction and normal AV conduction. The test was performed by pacing in the AAI mode and decrementing the atrial voltage amplitude at a pulse duration of 0.4ms
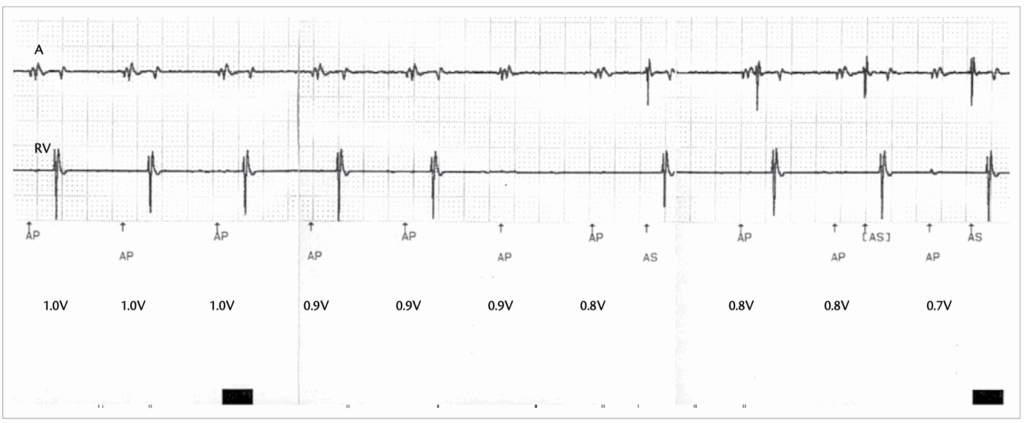
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 6
A 72-year-old patient with permanent AF and bradycardia had a single-chamber pacemaker implanted. The device was programmed to VVIR 60–120bpm. The rate response parameters were modified at follow-up, due to persistent breathlessness. She presented again, due to breathlessness and palpitations. Her rate histograms are shown here
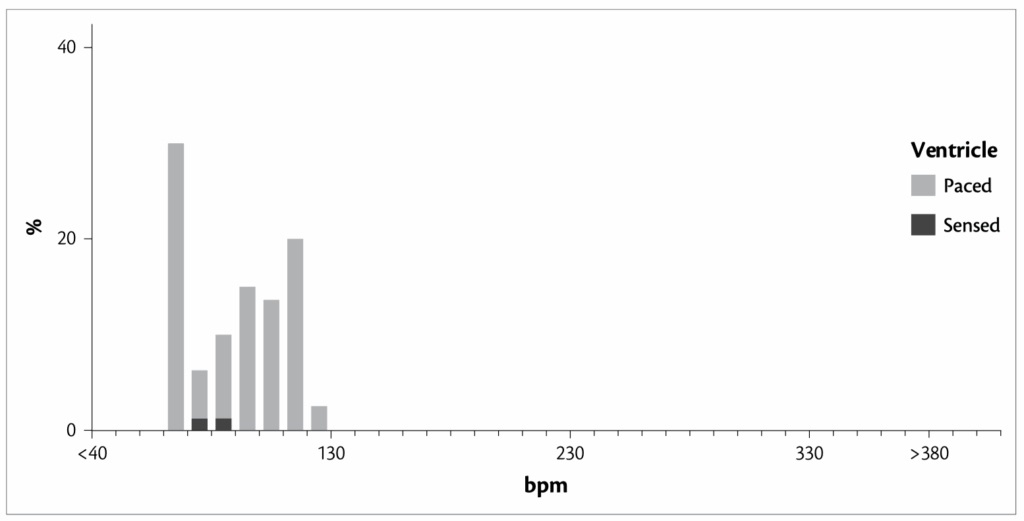
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
This proportion is too high for a patient of this age, implying that the sensor threshold is too low (i.e. too sensitive). The profile of the histogram shows an increasing proportion of events at an increasing heart rate, indicating that the sensor slope is too steep
Case 7
An 80-year-old woman implanted with a VDD pacemaker for complete AV block had recently undergone a generator replacement. She reported malaise, while carrying her shopping.
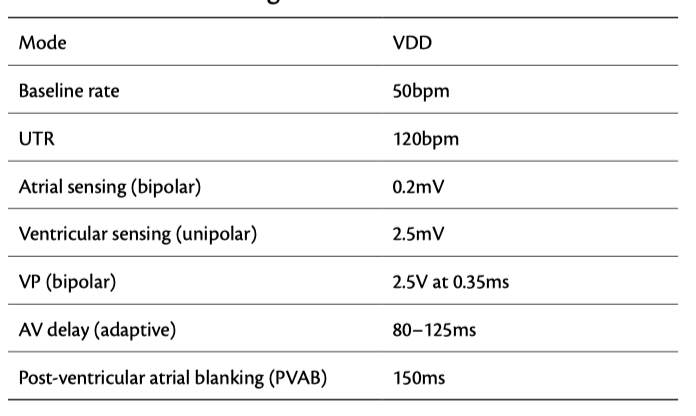

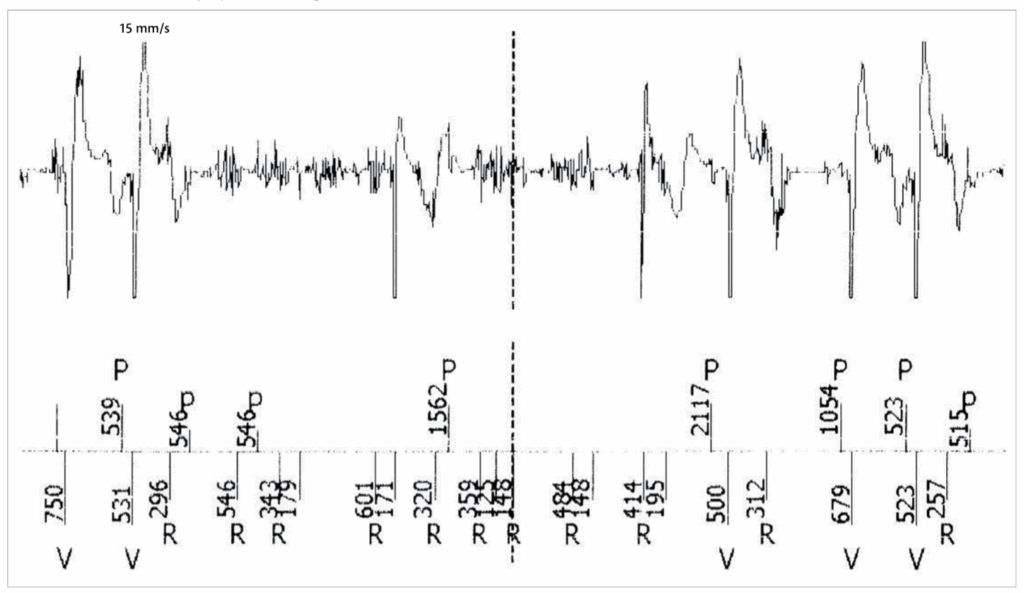
Ventricular oversensing here due to Pectoral myopotential
- Pectoral myopotential oversensing resulted from the unipolar sensing configuration and was confirmed by asking the patient to press her hands together, which reproduced the myopotential artefacts on the real-time EGM.
- Ventricular oversensing is a potentially lethal condition in pacemaker-dependent patients (as it may lead to asystole). The problem was corrected in this case by setting the ventricular sensing to a bipolar configuration.
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 8
A 72-year-old patient with complete AV block was followed by remote monitoring.
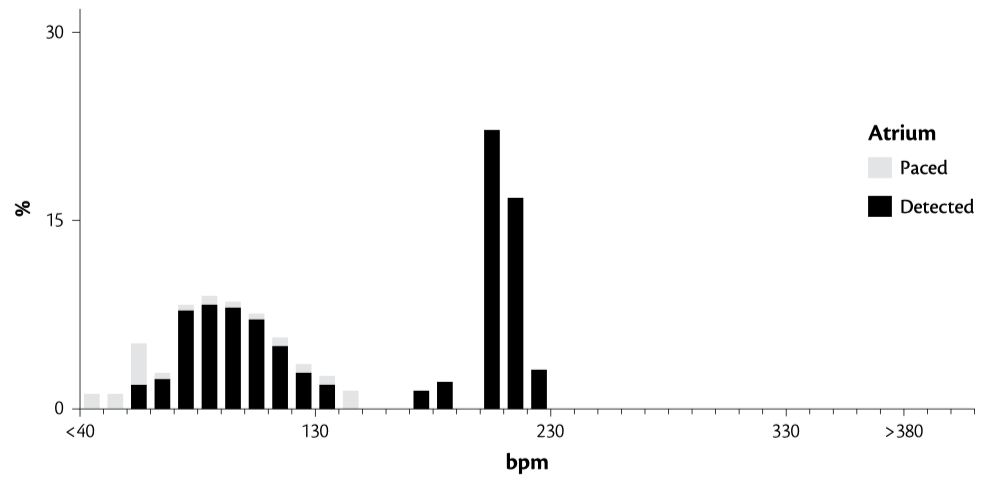
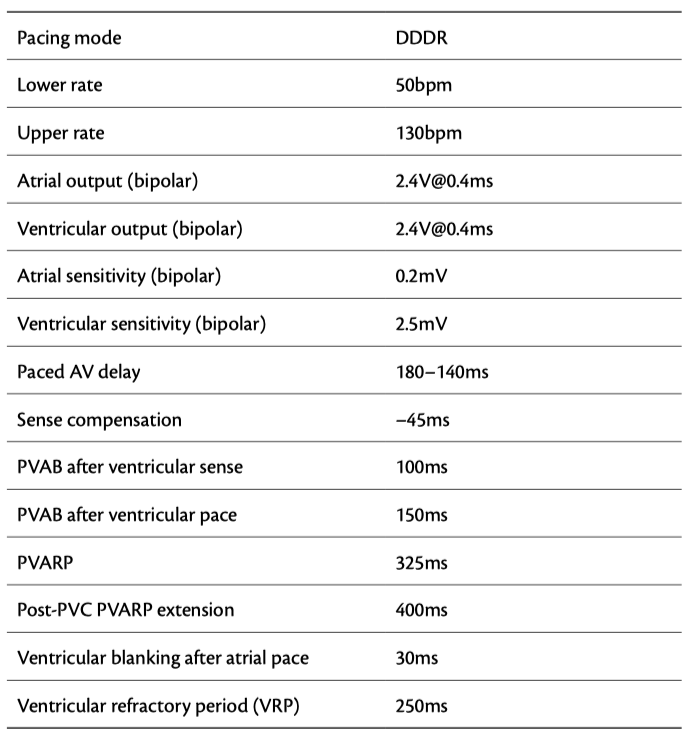
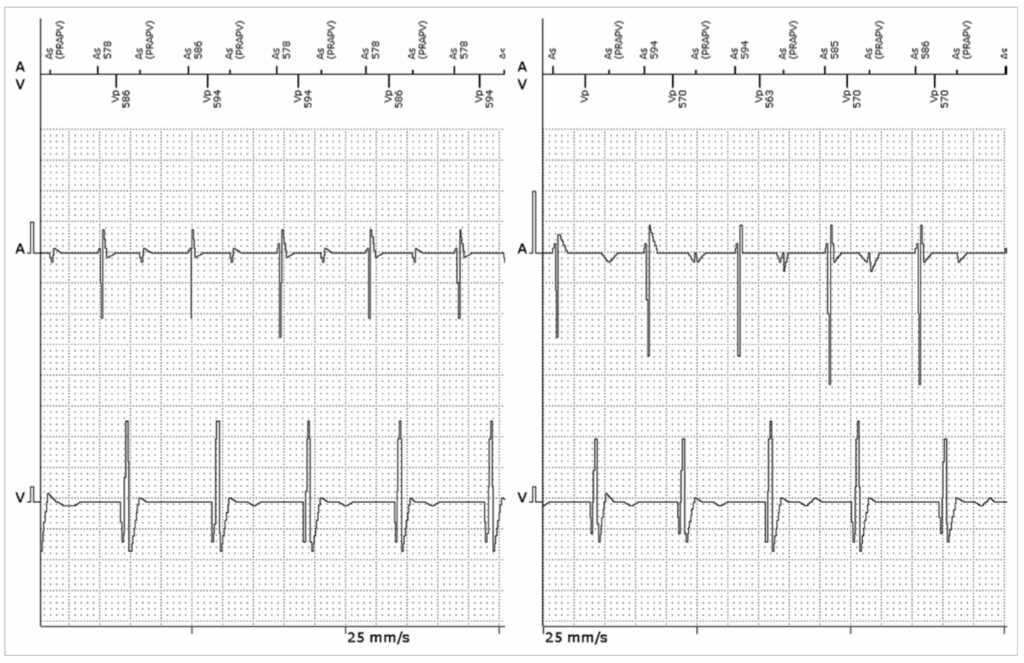
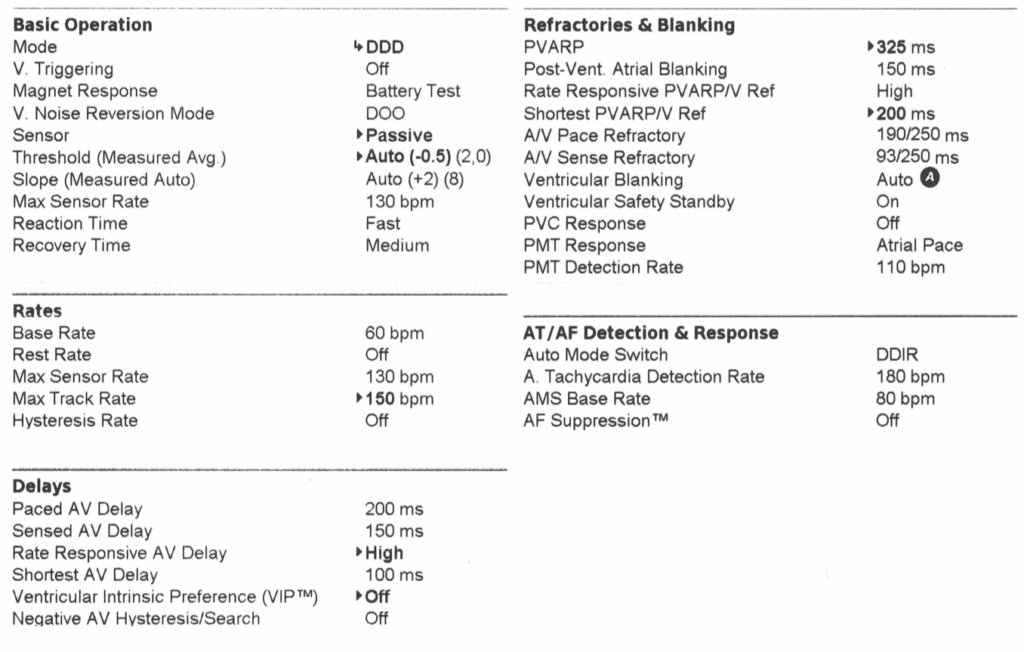
The device settings are shown in Table 10.1, and the atrial rate histogram is shown in Figure 10.1. High-rate atrial episodes were recorded, and the EGMs of two such episodes are shown here
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Far-field R-wave (FFRW) oversensing
A number of factors may favour FFRW oversensing:
- Proximity of the atrial lead to the ventricle
- Unipolar sensing configuration
- Programming a high sensitivity
- Short PVAB
- Inter-electrode spacing of the lead (with closer spacing, resulting in less FFRW oversensing).
The easiest way to correct the problem is to lengthen the PVAB, as was done in this case, from 150ms to 180ms. A more difficult issue to deal with is sensing of FFRW when it occurs before ventricular sensing. This occurs in about 25% of patients, especially in the setting of RBBB where the depolarization wavefront is sensed late into the QRS complex by the RV lead.
Case 9
A patient was implanted with a dual-chamber pacemaker for symptomatic Wenckebach AV block. A Holter was performed and is shown here
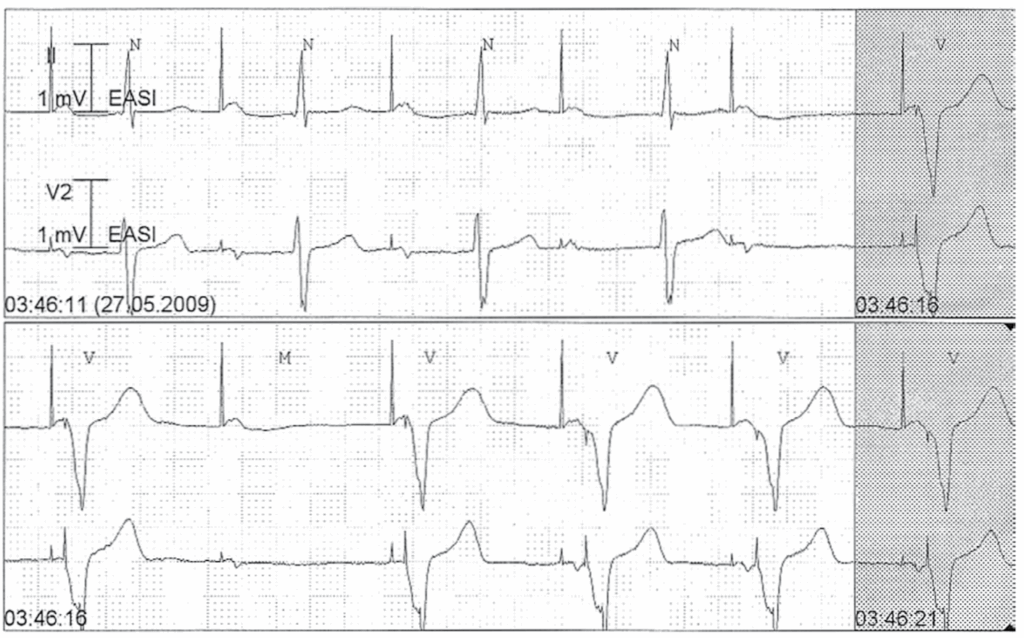
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
ADI switching to DDD
To avoid for patients with :
- Permanent complete AV block
- Patients with symptomatic first-degree AV block (as in the present case)
- Pacemaker-dependent patients who do not tolerate slow rates,
- Case of a long QT interval or history of torsades de pointes (due to the pro-arythmic effect of long-short sequences in this patients).
Case 10
A 72-year-old patient was implanted with a dual-chamber pacemaker for sick sinus syndrome, programmed with the ADIR/DDDR algorithm. His LVEF was normal. The device counters indicated 96% AP and 2% VP. He complained of persistent dyspnoea. A real-time EGM is shown & transthoracic echocardiogram was performed, and the transmitral Doppler flow is shown here
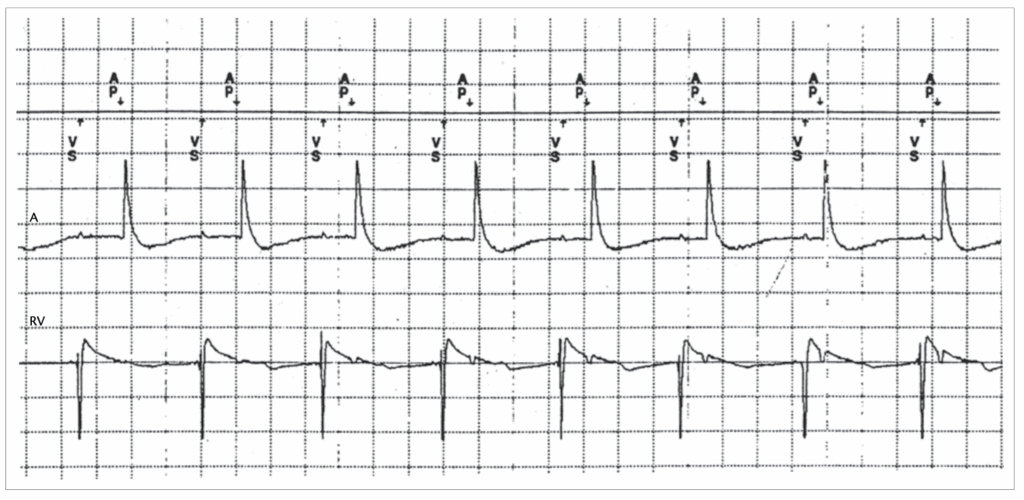
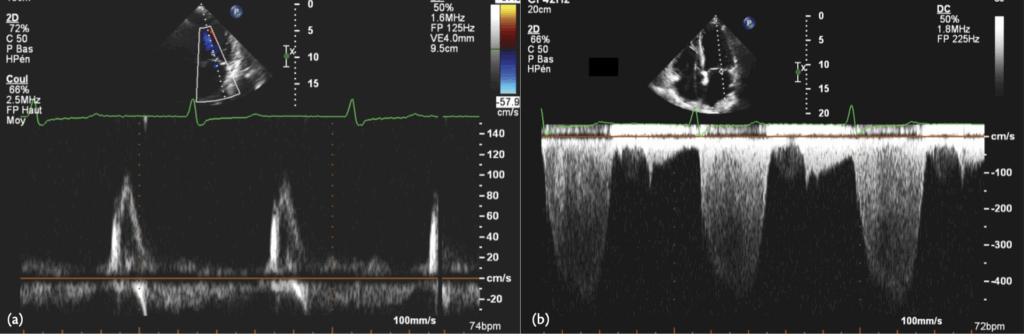
P on T’
The ADI/DDD algorithm tolerates very long AVIs, which may, as in this case, lead to ‘P on T’, with atrial contraction occurring during ventricular systole, as in the pacemaker syndrome. The detrimental haemodynamic effect of RV pacing in the DDD mode needs to be balanced against improved AV synchrony. In this case, programming the pacemaker to the DDD mode revealed improved ventricular filling (below), with the appearance of an A-wave, as seen below. Also, diastolic mitral regurgitation was eliminated, although it probably was not the main cause of the patient’s symptoms.
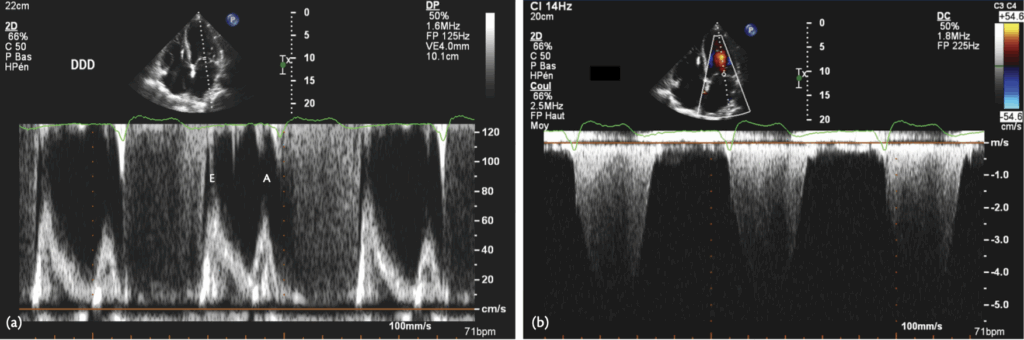
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 11
A 68-year-old patient was implanted with a DDDR pacemaker for sick sinus syndrome. He was asymptomatic. At follow-up, the episode retrieved from the device memory is shown here & the device settings
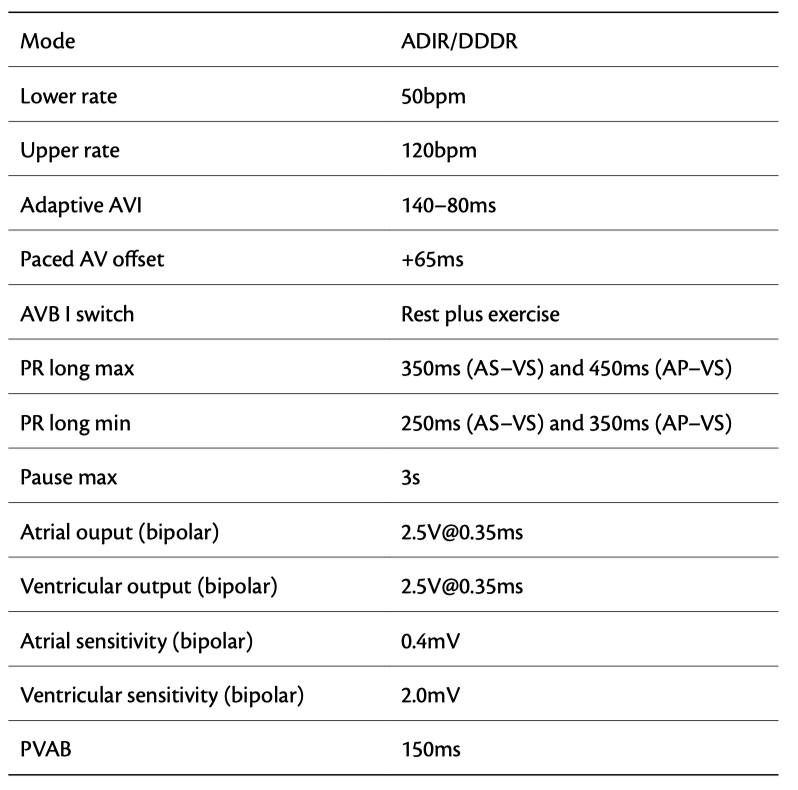
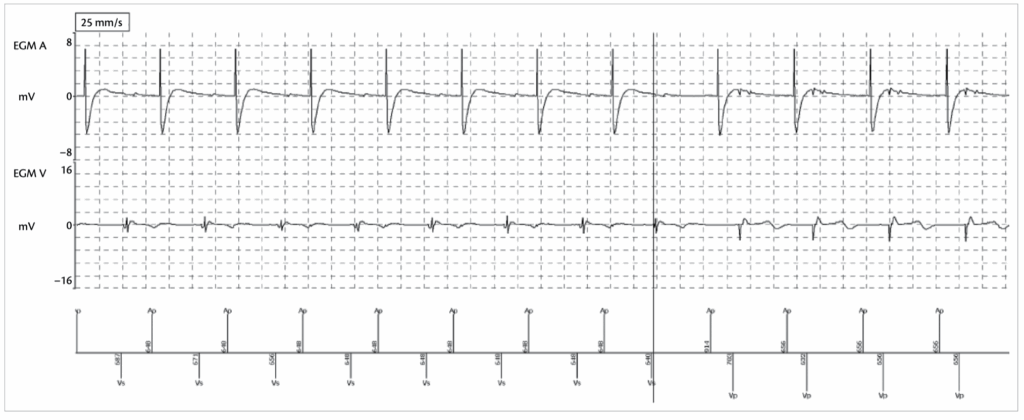
Avoiding ‘P on T’ with the ADI(R)/DDD(R) mode
This device has an evolved AV management algorithm that switches from ADI(R) to DDD(R), based upon three criteria:
- AV block (two consecutive or 3/12 blocked P waves)
- Ventricular pause (programmable to 2, 3, or 4s)
- Long PR intervals.
In order to avoid unduly long PR intervals that are usually allowed by the ADI(R)/ DDD(R) mode, this device has a first-degree AV block criterion. A maximum PR interval can be set (200–450ms, with the default value of 350ms and an additional 100ms for AP–VS intervals, as in this case). If six consecutive cycles have intervals which are greater than these thresholds, the device switches from the ADI(R) to the DDD(R) mode, in order to avoid the ‘P on T’ phenomenon observed before (case 10)
This is an EGM of the same patient …
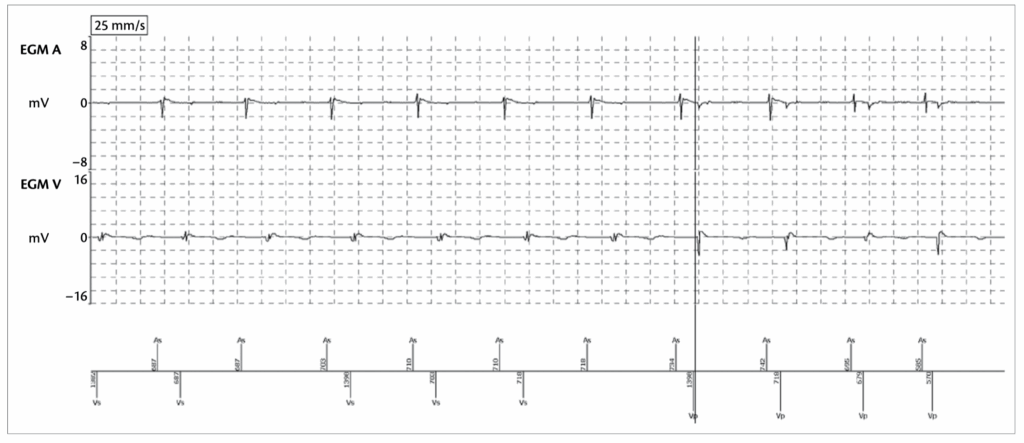
ADIR to DDDR mode due to ventricular undersensing -> AV block (two consecutive or 3/12 blocked P waves)
Do we need to change the ventricular lead ? -> Knowing that the VP is less than 1% & Here the histograms of sensing amplitude for conducted R-waves and PVCs
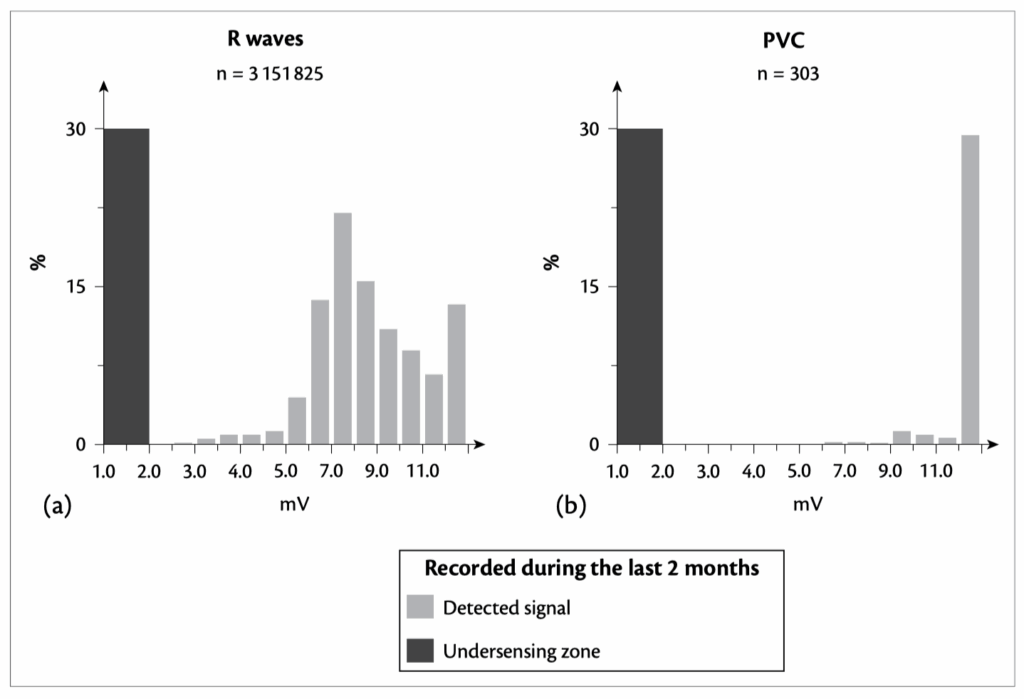
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Ventricular undersensing occurred rarely in this patient (few ADIR/DDDR mode switches were stored in the device memory, with <1% VP), and the histograms indicated that R-wave amplitude was usually satisfactory. The R-wave amplitude during device follow-up was measured at 8.2mV, but nevertheless the sensitivity was increased slightly from 2.0mV to 1.8mV.
Case 12

- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
DDI
1 – There is loss of AV synchrony with atrial sensed events (AS) at a constant ventricular pacing (VP) rate 60 bpm (VP-VP 996 – 1000 ms) -> this excludes DDD and VDD.
2 – In DDI mode -> VA interval is triggered after a VP or VS events. AR that fall within the PVARP do not inhibit AP.
3 – AP occurs at the end of the VA interval (800 ms).
4 – AV synchrony is maintained after AP events.
Pros :
– To avoid to programme very long AV delays in the DDD mode, to avoid RV pacing
– Atrial tachy-arrhythmias, to avoid rapid ventricular pacing
Cons :
– Asynchrony
Case 13
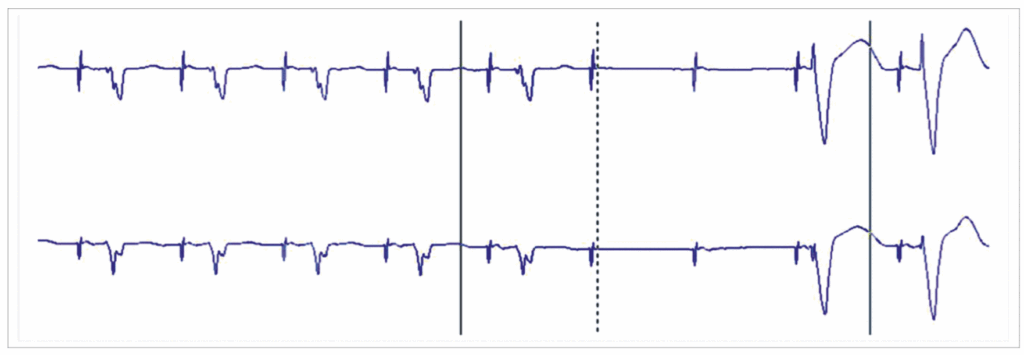
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
AV management algorithm
1 – You have 5 first cycles correspond to atrial pacing with intrinsic AV conduction
2- Than two cycles with AV blok (AAI)
3 – Than switch to DDD pacing
Case 14
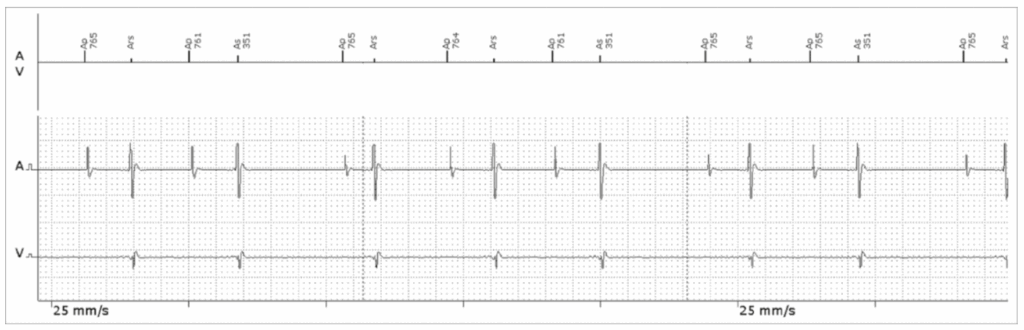
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Far Field R wave oversensing
Case 15
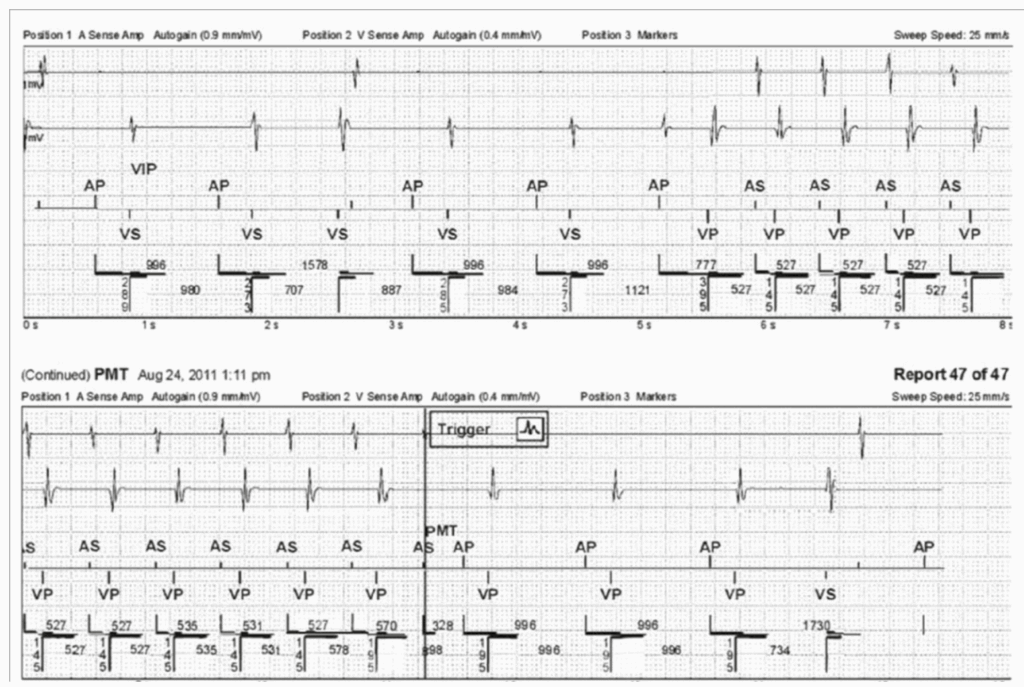
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
AV hysteresis
1 – VIP = ventricular intrinsic preference -> indicating that the current AV interval is longer than the programmed. This is due to AV hysteresis.
A PVC falls in the same time than the AP, the PVC falls in PAVB and is not seen, than AV timer trigger with a prolonged AV delay due to VIP than VP – retrograde VA conduction -> witch induce PMT
Case 16
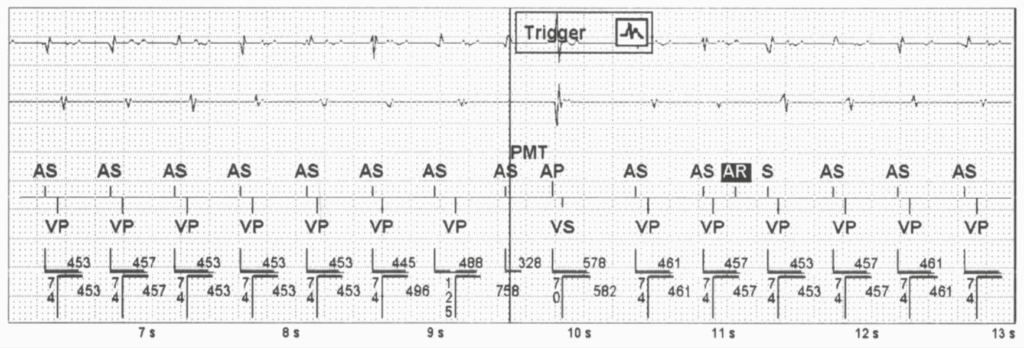
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Incorrect PMT diagnosis by the pacemaker
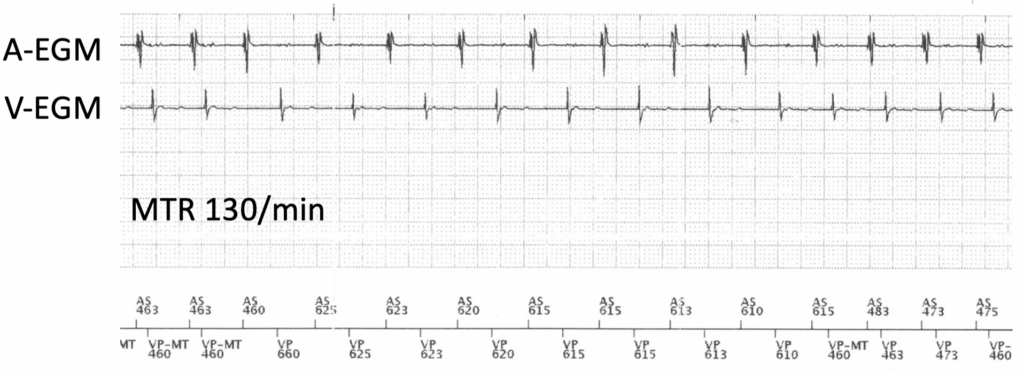
We see a sinus tachycardia above programmed PMT detection rate (130 bpm)
How to differentiate between SVT en Endless loop tachycardia
SVT VP-AS1 is different form VP-AS2 after extending AV interval
Endless loop tachycardia VP-AS1 is the same than VP-AS2 after extending AV interval
Case 17
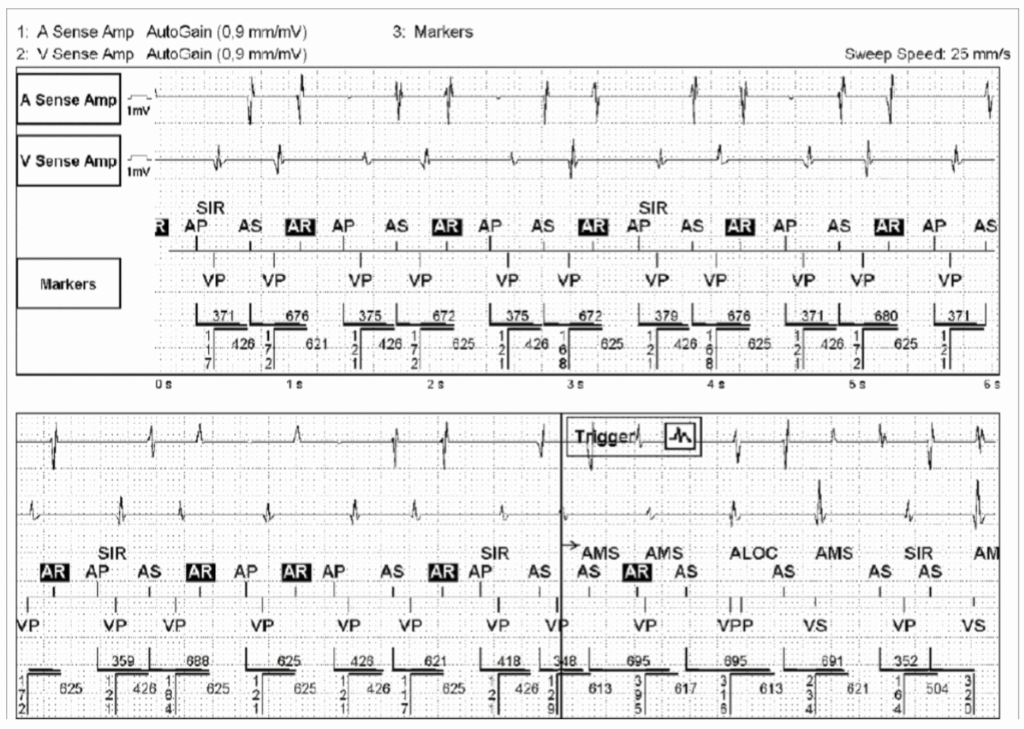
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Atrial bigeminy !
Case 18
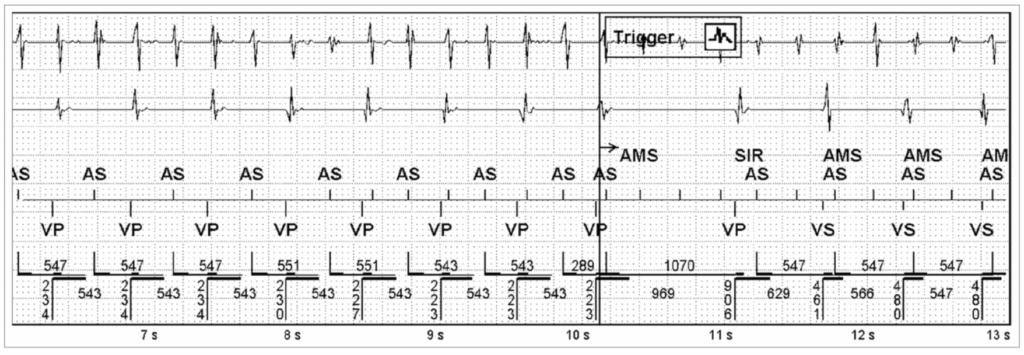
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Atrial Fuller lock in
Case 19
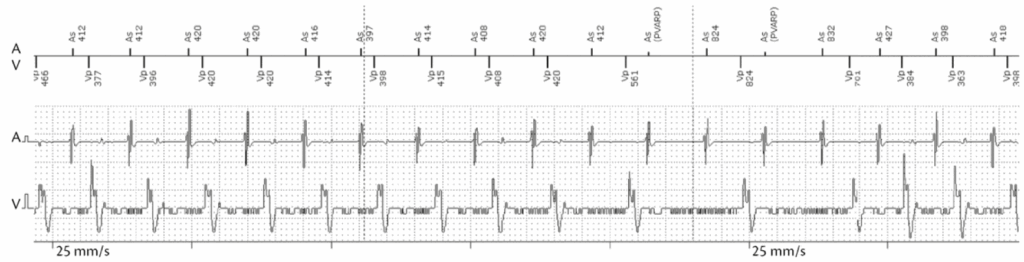
2:1 lock-in protection algorithm
- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
Case 20

- Reference : The EHRA book of Pacemaker, ICD and CRT Troubleshooting – Hasan Burri, Jean-Claude Deharo
2:1 lock-in protection algorithm
Case 21
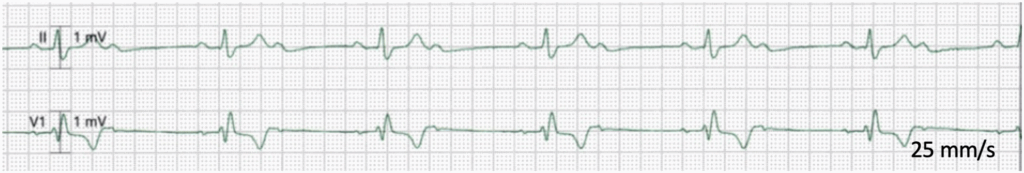
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
2:1 AV blok. Suggest Pacemaker implantation
Case 22

EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
200/min
Shortest PVARP : 200 ms + Shortest AV delay : 100 ms = 300 ms -> 60.000/300 = 200 bpm
Case 23
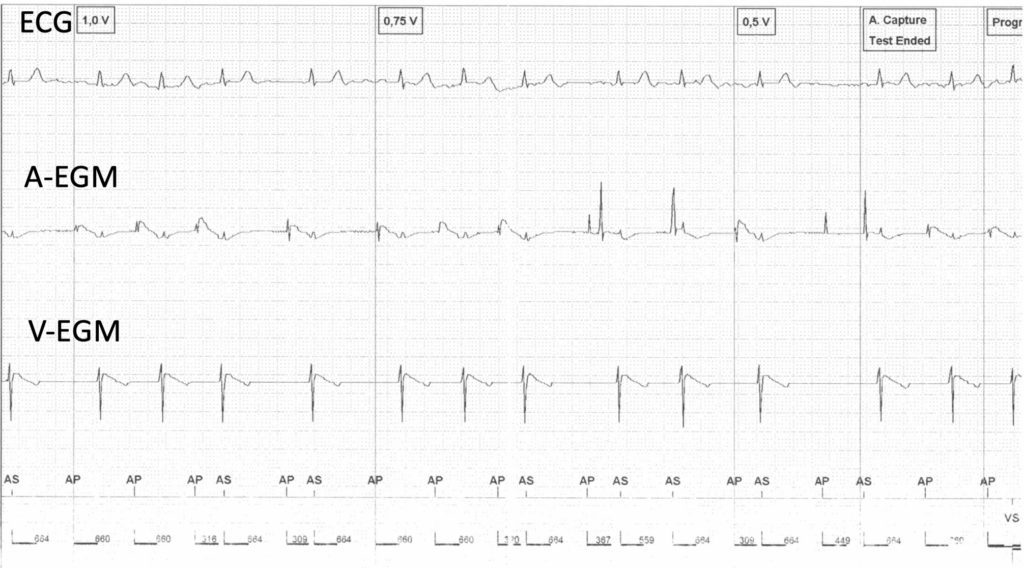
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
Case 24
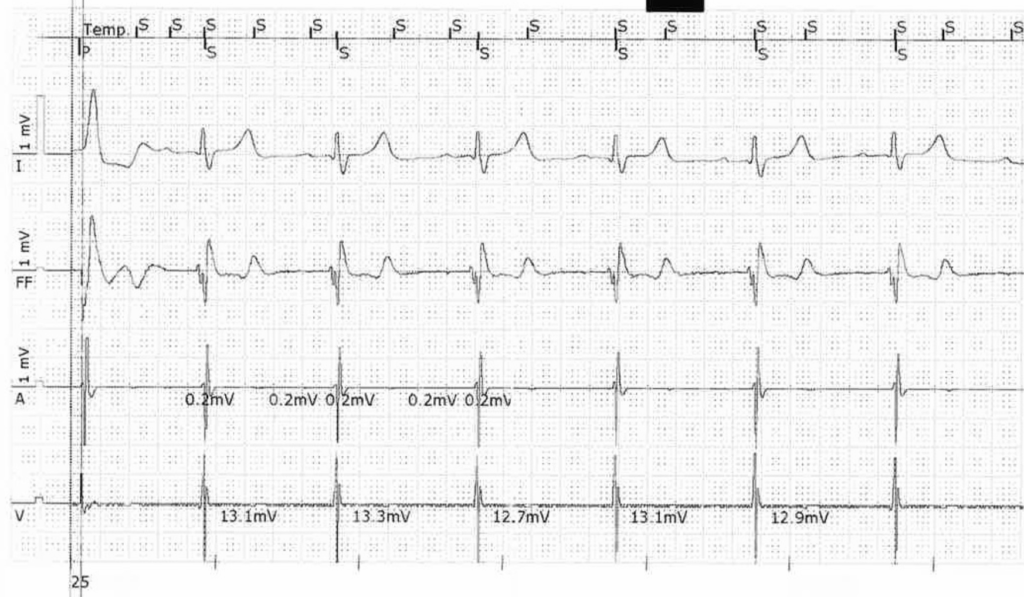
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
Atrial lead probably dislodged
Case 25
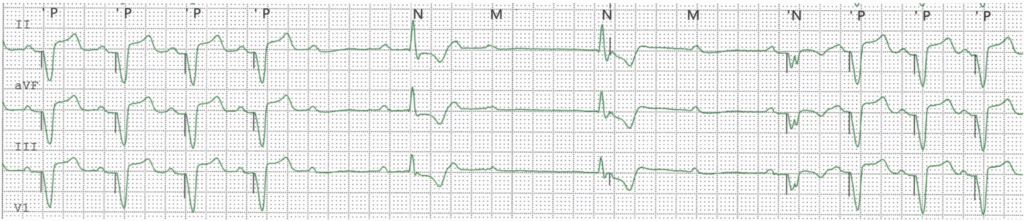
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
An algorithm to minimise ventricular pacing in action
Case 26
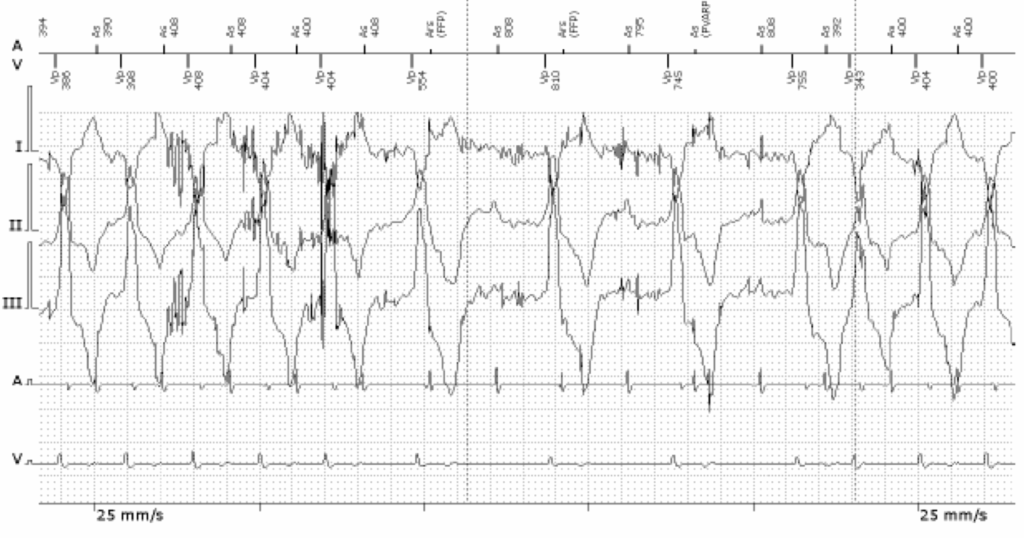
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
Case 27
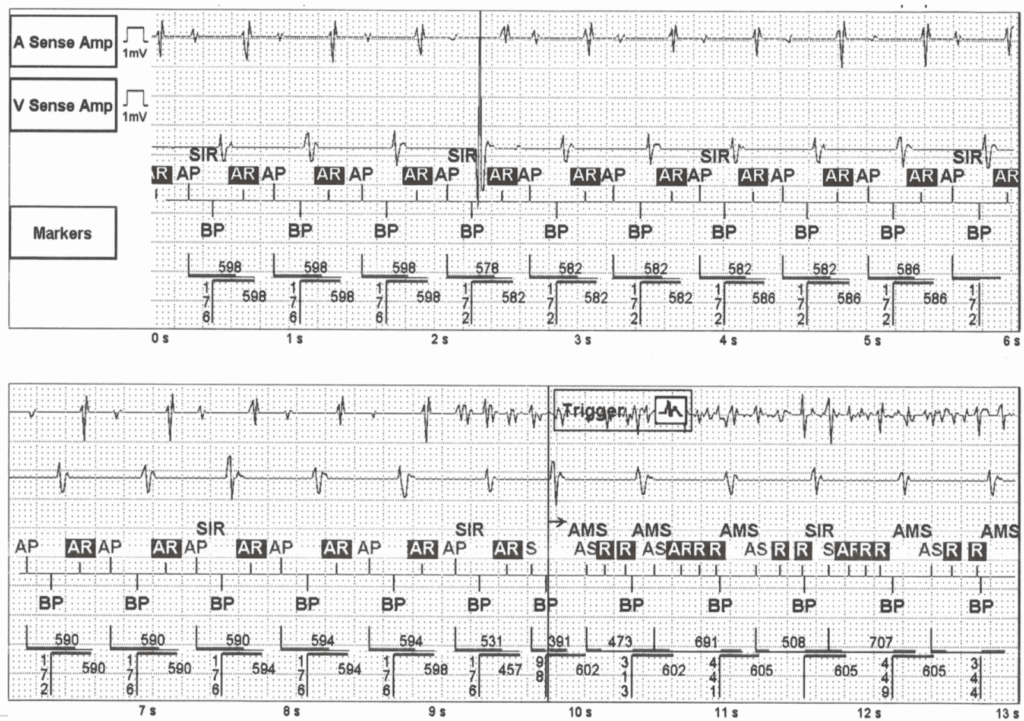
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
Probably a fracture of the atrial lead
Case 28
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
Torkel Steen, MD, PhD
Sinus tachycardia and search AV delay algorithm in action
Case 29
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
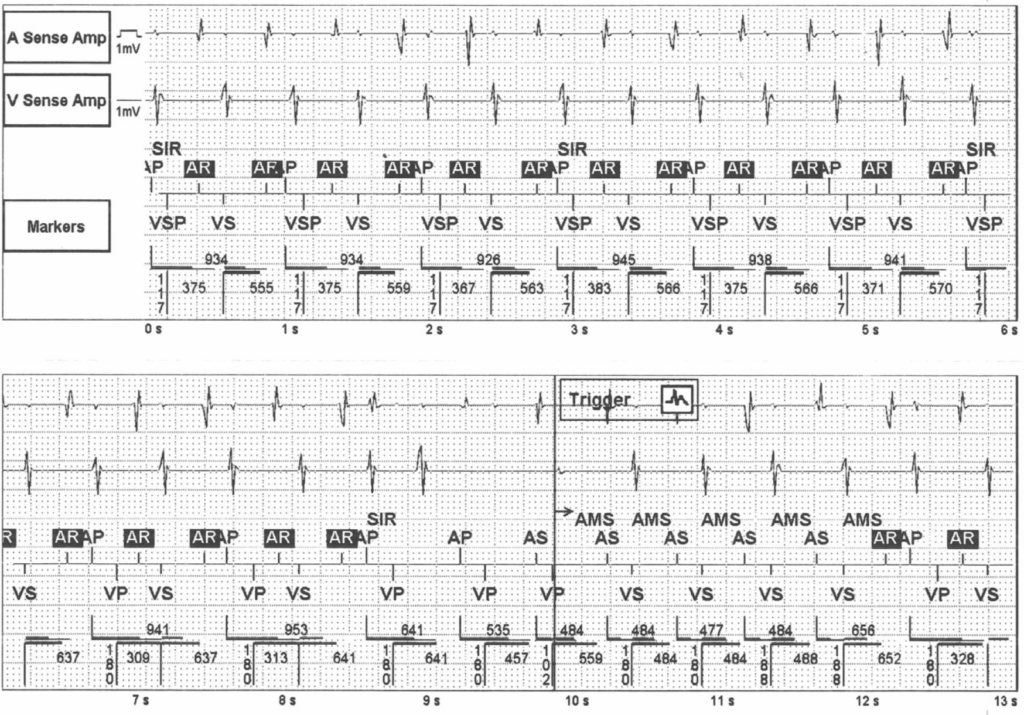
Torkel Steen, MD, PhD
RNRVAS gives modeswitch
Case 30
EHRA Course on Cardiac Pacing, ICD and Cardiac Resynchronisation Therapy Vienna, June 2025
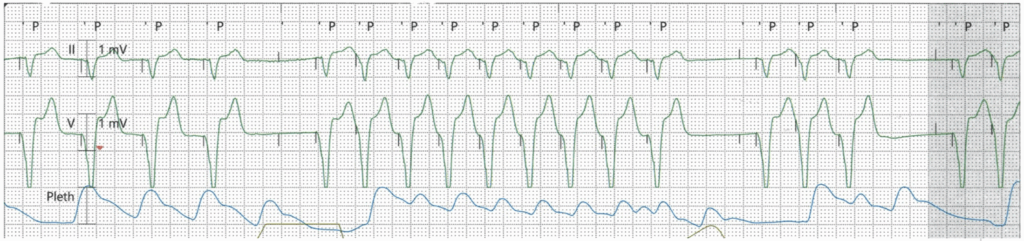
Torkel Steen, MD, PhD
AV search hysteresis and PMT termination algorithm